Southern California University of Health Sciences (SCU) and Pacific College of Health and Science (PCHS) today jointly announced that they have signed a definitive agreement through which SCU will assume PCHS’s Chicago and San Diego campuses and programs …
Continue reading “Chicago and San Diego Campuses of Pacific College of Health and Science (PCHS) to join Southern California University of Health Sciences (SCU)”
From January 2023 through July 2023, Dr. Leng Tang-Ritchie represented Pacific College in the development of the Women’s Health Innovation Opportunity Map, sponsored by the Bill & Melinda Gates Foundation and the US National Institutes of Health (NIH). Leng Tang-Ritchie is our Vice President of Clinical Education and Operations. Women’s health is an area that …
Continue reading “Dr. Tang-Ritchie Represented PCHS at the 2023 Women’s Health Innovation Opportunity Map”
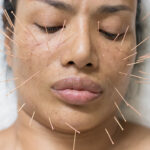
Sandra Lanshin Chiu, LAc, MSTCM, a PCHS alum who earned her acupuncture master’s from our New York campus in 2005, was recently interviewed by Katie Baxter for an article on cosmetic acupuncture in Well+Good, a publication that reports upon and highlights wellness and lifestyle trends. “Over time, Chinese medicine developed to treat all kinds of …
Continue reading “Sandra Chiu, Pacific College Alum, Interviewed by Well+Good on Cosmetic Acu”
Pacific College holistic nursing faculty members Mitzie Meyers, PhD, RN, CNE, AHN-BC and Caroline Ortiz, PhD(c), MSN, MPH, RN, NC-BC were recently interviewed for an article series by Andy Oram on problems people have taking their medication. Up to half of all patients who are prescribed medications for management of chronic conditions don’t take them …
Continue reading “Problems with Prescribing Medication: Pacific Faculty Interviewed by Healthcare IT Today”
Pacific College holistic nursing faculty members Mitzie Meyers, PhD, RN, CNE, AHN-BC and Caroline Ortiz, PhD(c), MSN, MPH, RN, NC-BC were recently interviewed for Healthcare IT Today’s article “Rethinking Medication and Information Technology”, the fourth and final part in a series by Andy Oram on problems people have taking their medication. Many patients who have …
Continue reading “Rethinking Medication: Holistic Nursing Professors Interviewed by Healthcare IT Today”
Mitzie Meyers, PhD, RN, CNE, AHN-BC, a professor in Pacific College’s nursing program, was recently interviewed for Healthcare IT Today’s article “What Tends to Go Wrong With Medication Adherence?”, the third in a series by Andy Oram about problems people have taking their medication. Many patients prescribed medications for management of chronic conditions don’t take …
Continue reading “Mitzie Meyers, Pacific College Faculty, Interviewed by Healthcare IT Today”
Caroline Ortiz, PhD(c), MSN, MPH, RN, NC-BC, an associate professor in Pacific College’s nursing program, was recently interviewed for Healthcare IT Today’s article “Helping People Take Their Meds”, the second in a series by Andy Oram about problems people have taking their medication. Up to half of all patients who are prescribed medications for management …
Continue reading “Caroline Ortiz, Pacific College Faculty, Interviewed by Healthcare IT Today”
Dr. Cynthia Neipris, DACM, LAc, Pacific College’s Vice President of Alumni Services and Director of Outreach and Community/Continuing Education as well as faculty on the New York campus, was recently elected ACAHM Commissioner as an At-Large member. The Accreditation Commission for Acupuncture and Herbal Medicine (ACAHM) is a specialized agency recognized by the United States …
Continue reading “NY’s Cynthia Neipris Elected ACAHM Commissioner”
Dr. David R. Sol, DAc, LAc, LMT, CFMP, the Dean of Undergraduate Studies at Pacific College of Health and Science’s Chicago campus, was extensively cited in a recent article by Lauren David, writing on post-workout massage for Verywell Fit, an award-winning resource for nutrition and exercise information. Most people know that stretching can help prevent …
Continue reading “Chicago’s David Sol Cited by Verywell Fit on Post-Workout Massage”
The Herbal Highway, a podcast and radio show, recently interviewed Dr. Leng Tang-Ritchie, Vice President of Clinical Education and Operations and Director of Clinical Services at Pacific College of Health and Science, for an exploration of emotional health and balance from a Chinese medical perspective. During the course of the hour-long conversation, Dr. Tang-Ritchie dove …
Continue reading “Herbal Highway Interviews Tang-Ritchie on Chinese Medicine”
Natural Practitioner recently included Chava Weinberg, DACM, LAc, LMT, department chair and clinical supervisor on Pacific College’s New York campus, on a panel of experts discussing the causes of and natural treatments for pain and inflammation. Natural Practitioner is an industry trade magazine that provides health, nutrition and business information to integrative health care professionals …
Continue reading “Natural Practitioner Interviews Chava Weinberg, Dept Chair, on Pain and Inflammation”