Acupuncture School
Next term starts on May 4th, 2026!Pacific College's Acupuncture School
 Over the past 50 years, acupuncture and other similar East Asian modalities such as herbology or tui na bodywork have increasingly gained in popularity. In fact, they have evolved into one of the most utilized forms of complementary integrative medicine interventions in the United States. According to the National Institute of Health (NIH)*, more than 10 million acupuncture treatments are administered annually in the United States alone. This rise in popularity can be attributed in part to its effectiveness for pain relief, nausea, allergies, and other chronic and acute conditions, and in part to the fact that scientific studies have begun to prove its efficacy.
Over the past 50 years, acupuncture and other similar East Asian modalities such as herbology or tui na bodywork have increasingly gained in popularity. In fact, they have evolved into one of the most utilized forms of complementary integrative medicine interventions in the United States. According to the National Institute of Health (NIH)*, more than 10 million acupuncture treatments are administered annually in the United States alone. This rise in popularity can be attributed in part to its effectiveness for pain relief, nausea, allergies, and other chronic and acute conditions, and in part to the fact that scientific studies have begun to prove its efficacy.
Since 1986, Pacific College has led the movement and trained dedicated practitioners with graduate degrees in acupuncture and Chinese medicine. We tirelessly advocate for research and regulation, and even offered the very first doctorate completion program for acupuncturists holding a master’s degree back in 2016. Today, as acupuncture continues to grow as a non-pharmaceutical, adjunct modality to conventional allopathic medical treatments, the demand from patients and their loved ones is increasing, and acupuncture is now offered even at prestigious academic medical centers.
Pacific College's Acupuncture and Chinese Medicine Programs

Click on any of the program names below to learn more!

Students who attend Pacific College’s acupuncture programs also receive training in the practice of therapeutic exercise such as qigong, Eastern body therapy such as tui na massage, as well as Chinese herbology and nutrition.
(*) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4104560
Acupuncture Schools at Pacific College of Health and Science

(*) Former DACM program name was changed in accordance with the new policy established by the Accreditation Commission for Acupuncture and Herbal Medicine (ACAHM). However, the curriculum remains the same.
(**) Former MSTOM program name was changed in accordance with the new policy established by the Accreditation Commission for Acupuncture and Herbal Medicine (ACAHM). However, the curriculum remains the same.
Acupuncture Degree and Certification Highlights
Develop professional skills through hands-on experiences in on-campus clinics
Learn from experienced acupuncturists
Apply techniques taught in the classroom in Pacific College’s externship program
Join the local community in annual health and wellness events
Find financial aid options and create your own flexible schedule
Pacific College is the largest accredited acupuncture school
Become eligible for state licensure exams
Acupuncture programs at acupuncture school
This program makes students eligible for the California state licensure exams as well as the national certification examinations, which enable students to become licensed in the remaining states that regulate acupuncture colleges and Chinese medicine schools.
This program helps students become eligible for the national certification examinations from NCBAHM and allows the student to become licensed in states that regulate acupuncture and Chinese medicine using the NCBAHM exam. As this program does not require herbology, it’s a shorter duration than the MSAcCHM.
The program has been designed for licensed acupuncturists and qualifies students to become eligible for the NCBAHM exam in Chinese Herbology.
The Pacific College of Health and Science has designed this pathway for acupuncturists who already have their master’s (or equivalent) to continue their work and receive their doctorate.
Acupuncture School Admissions Requirements
The following list outlines common prerequisites:
- Educational Background. Most schools of acupuncture require applicants to have a high school diploma or equivalent. Some programs may also look for individuals with a background in healthcare or related fields.
- Transcripts and GPA. Applicants to acupuncture colleges or schools are usually required to submit their academic transcripts from previous educational institutions. A competitive GPA may strengthen the application.
- Prerequisite Courses. Some schools may ask students to complete specific prerequisite courses, such as biology, anatomy, or psychology, before enrollment.
- Letters of Recommendation. Acupuncture programs often request letters of recommendation from teachers, employers, or healthcare professionals who can vouch for the applicant’s dedication and suitability for the program.
- Admission Test. A standardized admission test might be required. This test assesses the applicant’s knowledge and aptitude for the program.
In some cases, in order to receive training in acupuncture, candidates may need to participate in an interview with faculty members to demonstrate their passion for acupuncture and their commitment to the profession.
Highlights of the Acupuncture Program
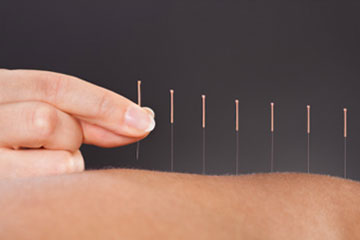
Acupuncture schools provide in-depth and comprehensive acupuncture training programs in the principles and techniques of acupuncture. In these acupuncture classes, students learn about meridians, acupoints, and how to stimulate the body’s natural healing processes through this ancient practice. What else can the program offer?
- Practical Experience. Most acupuncture programs emphasize hands-on training, giving students ample opportunities to practice their needling skills under the guidance of experienced instructors. This practical experience ensures that graduates are well-prepared to begin their careers confidently.
- Holistic Approach. Acupuncture’s foundation in Traditional Chinese Medicine means that students attending acupuncture classes also gain insights into other TCM practices, such as herbal medicine and cupping therapy. This holistic approach equips practitioners to address a wide range of health concerns and promote overall well-being.
- Patient-Centered Care. Acupuncturists often build strong relationships with their patients, as they focus on understanding individual health needs and crafting personalized treatment plans. This aspect of the practice can be deeply rewarding for those who value a patient-centered approach.
With the increasing interest in alternative medicine and holistic health, the demand for qualified acupuncturists who have finished school for acupuncture is on the rise. As people seek natural and non-invasive healing methods, acupuncturists play a crucial role in meeting this demand.
Is a Career in Acupuncture Right For You? Find Out!
This fun, online quiz takes 3 minutes to complete and you’ll receive a personalized report. Identify your strengths and social style to help you determine what you are best suited for. Get your Acupuncture Career Readiness score now!
Why Acupuncture School?
Acupuncture education is becoming increasingly significant in the U.S. as an estimated 20 percent of the population seeks relief from lower back pain. This traditional treatment approach has garnered widespread recognition among healthcare professionals and is gradually becoming a key part of holistic healing. The growing appeal of acupuncture has, in turn, spiked the demand for well-trained acupuncturists with a solid foundation in both biomedicine and holistic healing.
The acupuncture programs offered at Pacific College furnish students with an education deeply rooted in Eastern holistic healing practices and Western biomedical science. The acupuncture school contributes significantly to the holistic care field, equipping students for lifelong careers in this alternative treatment. Acupuncture schooling, such as that provided by Pacific College, forms an integral part of the evolving healthcare landscape. The colleges of acupuncture like Pacific College play an essential role in fostering and molding future practitioners, preparing them for rewarding careers in the realm of holistic and alternative healthcare.
Who Should Choose an Acupuncture College?
As the desire for holistic treatments and alternative healthcare options expands in the U.S., acupuncture is gaining considerable traction, especially among enthusiasts of natural and organic lifestyles. With an acupuncture training program specifically tailored to these needs, the School of Acupuncture at Pacific College is reaching out to these individuals, and all others keen on understanding and promoting the natural balance within the human body.
The learning acupuncture experience we offer has been carefully curated for those seeking to transform their fervor for health and wellness into a fulfilling career in acupuncture. At Pacific College, our acupuncture classes skillfully fuse the principles of modern biomedicine with time-honored holistic healing practices. This blend draws on the strengths and effectiveness of both realms, offering a comprehensive foundation for our acupuncture programs.
Those participating in our courses will not just learn acupuncture, but also gain an in-depth understanding of the therapeutic potential that lies within this age-old Chinese medicinal practice. This innovative learning approach positions Pacific College as a leading choice for individuals pursuing a career in the evolving field of acupuncture.
Recently, CNS Neuroscience and Therapeutics published a review that proposed acupuncture as a comparable alternative to using cognitive-behavioral therapy to treat anxiety. More and more health practitioners are advocating for the expansion of the practice of acupuncture, and the role of Chinese medicine within the Western healthcare landscape will play a heavier role in shaping future perspective on holistic care. The acupuncture courses at the Pacific College acupuncture school were designed to challenge and motivate students to grow personally and professionally to become leaders within their local communities.
Student Testimonial About Acupuncture School
“Pacific College gave me a foundation for a limitless future in the field of holistic healing and acupuncture. I feel that I gained an authentic and deep understanding of holistic medicine during my time at Pacific, and I now feel like I can have a truly rewarding acupuncture career.”
-Eric Brand
Acupuncture Career Outlook
It is estimated that 35 million Americans undergo acupuncture treatments regularly, and this trend is growing as acupuncture becomes increasingly accepted by medical insurances as a treatment for pain and other chronic conditions. In addition, acupuncturists are now also working alongside traditional medical practitioners to deliver multidisciplinary care programs for people with a wide range of conditions. As a result, there’s never been a better time to choose a career in acupuncture.
According to the US Bureau of Labor and Statistic, the discipline is expected to grow faster than average, by 5 percent, in America between 2022 and 2032.
As of 2022, roughly 26,600 licensed acupuncturists work in spas, cancer clinics, physical therapy and chiropractic offices, hospitals, educational institutions, and national and state agencies. The demand for acupuncturists is set to increase, partly due to new clinical studies that highlight acupuncture as an effective alternative treatment for pain.
How much does Acupuncture School cost?
Students interested in TCM schools should also consider other expenses, such as textbooks, supplies (e.g., acupuncture needles), and living costs if they are moving to attend school. Financial aid, scholarships, and grants may be available to help offset these costs for eligible students.
Pursuing a career in acupuncture and getting the necessary acupuncture training can lead to a gratifying and meaningful journey in alternative medicine. Acupuncture schools offer comprehensive training, practical experience, and a patient-centered approach to healing. By meeting the admission requirements and considering the cost of attending an acupuncture program, aspiring acupuncturists can embark on a fulfilling path to becoming certified professionals in this ancient healing art.
Acupuncture College Tuition
The tuition costs for the different acupuncture programs vary. You can see a breakdown of all the costs for each course and for the complete acupuncture school tuition and fees by visiting the college catalog.
Start a Rewarding Career in Acupuncture with Our Programs
Start your journey towards a rewarding career in acupuncture through our comprehensive acupuncture programs. At Pacific College, we stand as one of the premier accredited acupuncture schools, offering an exceptional education that paves the way for an esteemed acupuncture degree.
Our distinguished programs provide a holistic approach to acupuncture education, blending traditional wisdom with modern techniques, allowing our students to become masters of acupuncture. By enrolling at Pacific College, you’ll gain access to experienced faculty, modern facilities, and a supportive learning environment. Our commitment to excellence ensures that you’ll receive a quality education, setting you on a path to success in the field of acupuncture.
Choose Pacific College for its renowned reputation, accredited curriculum, and the advantage of a transformative acupuncture education that will empower you to make a meaningful impact on the well-being of others.
ABOUT PACIFIC COLLEGE OF HEALTH AND SCIENCE
Since 1986, those with a calling to heal and promote overall health in the mind and body have been led to the programs at Pacific College of Health and Science. Graduates are prepared to both prevent and remedy pain, discomfort, and disease through practices such as massage therapy, acupuncture, and holistic nursing.
Pacific College prepares students for careers as healing practitioners through an intersection of Eastern healthcare practices and Western bioscience with a strong hands-on clinical component. All three campus locations feature student clinics where learning practitioners serve the needs of real clients.
Acupuncture School FAQS
How does acupuncture work?
What does acupuncture treat?
Is acupuncture safe?
Is acupuncture school worth it?
How long is acupuncture school?
How much is acupuncture school?
Ready to Apply?
If you think a career in acupuncture is something you would like to pursue, contact us and speak to an admissions representative to get started on your new journey!
For more information, call (855) 866-6767 or fill out our contact form to be contacted by a Pacific College representative.